PUBERTY
PROBLEMS AT SCHOOL?
STOPPED EATING?
PREVENT / MANAGE CRISES
THE NEED FOR A SPECIALIZED ADOLESCENT MEDICINE

GROWTH DURING PUBERTY
BUCH TAB
The PEZZ Growth Atlas is also available as a book from PEZZ Publishing.
WHEN BODY AND MIND ARE CHANGING
Pubertal development usually begins in girls between 9 and 13 years of age and in boys between 11 and 15 years. However, it can also start earlier or later, be too early or too late, or not occur at all. In some adolescents, medical evaluations and, if necessary, treatment may be required.
Puberty involves biological, psychological, and social changes, which are often experienced as stressful or crisis-like. Psychosomatic complaints are also common. At the Pediatric Endocrinology Center Zurich, uncertainties that may arise during pubertal and adolescent development are addressed and reduced through professional counseling. This helps adolescents manage crises and ensures that psychosomatic complaints are treated effectively.
Emotional well-being and the associated psychosocial development are significantly influenced by short stature or by early or late onset of puberty. This, in turn, can lead to changes in social behavior and academic performance. At our center, young patients are, if needed, also counseled by psychologists specialized in pubertal issues.

PUBERTAL DEVELOPMENT
IN GIRLS
In girls, pubertal development typically begins around the age of 11 with breast development, the growth of pubic hair, and an acceleration of growth. The first menstrual period usually occurs around age 13. By age 15, growth is generally complete, and fertile cycles become more regular, reflected in a consistent menstrual cycle.
IN BOYS
In boys, puberty typically begins around age 13 (about 2 years later than in girls) with enlargement of the testes and the growth of pubic hair. Between ages 14 and 15, puberty reaches its peak: growth velocity is maximal, the voice breaks, and the first ejaculation occurs. By age 17, growth and pubertal development are generally complete.

WHEN SHOULD FURTHER EVALUATION BE DONE?
BUCH TAB
In the article Normvarianten und Pathologien der Pubertätsaentwicklung Dr. med. Claudia Katschnig explains that identifying disorders requires solid expertise.
You can also read the article in Beobachter from the 23rd of November 2018
TOO EARLY, TOO LATE?
Early onset of puberty that may require medical evaluation and possibly treatment is defined as the start of pubertal development before the age of 8 in girls and before the age of 10 in boys. Puberty is considered delayed in girls if there are no signs of breast development by the age of 13, or if the first menstrual period has not occurred by the age of 15. In boys, the first signs of puberty are often more subtle. However, if no visible pubertal development has started by the age of 16, a medical assessment is recommended.
Boys in particular who develop later than their peers often struggle with the delay, as they may still look childlike at the age of 15 and are therefore frequently teased. It is important to know that for so-called late developers there are simple treatment options that can help accelerate delayed pubertal development and, consequently, growth.
MORE
Regardless of issues relating to growth and physical changes, the psychological development that occurs during adolescence presents a major obstacle for young people and their parents. In such cases, specialist psychological guidance and counselling can often be very helpful.
ANOREXIA
During puberty, both the body and the mind undergo significant changes. Anorexia reflects the complex and often troubled relationship between body and mind. We also have extensive experience in the care of patients with anorexia. The primary goal of treatment is to help patients return to a minimum healthy weight as quickly as possible without the need for hospitalisation and to prevent serious complications.

THE NEED FOR A SPECIALIZED ADOLESCENT MEDICINE
ADOLESCENTS ARE NEITHER BIG CHILDREN NOR SMALL ADULTS.
They have their own specific needs. Marketing strategists in the clothing industry recognized this long ago and generate substantial revenues with products specifically targeted at adolescents. However, adolescents also have distinct needs when it comes to medical care, which differ from those of children and adults. In Switzerland, with only a few exceptions, there are no specialized practices or institutions dedicated to this age group.
WHY HAVE ADOLESCENTS SUDDENLY BECOME SO IMPORTANT?
The group of adolescents has grown significantly in recent years. Two opposing developments are responsible for this: sexual maturity occurs increasingly earlier, while the period of education and training has become progressively longer. At the beginning of the 20th century, in many professions such as factory work or farming, the onset of sexual maturity marked both the beginning and the completion of the transition into the adult working world. Most occupations at that time primarily required people to have their full physical strength available. This strength, however, already approaches its peak at the time of sexual maturity.
MORE
Today, sexual maturity occurs significantly earlier, while full integration into a profession as an adult comes increasingly later. Hardly any apprentice achieves full professional recognition before the age of 20. This phenomenon is even more pronounced among university students. A clear example can be seen among aspiring physicians: a young doctor is only recognized as fully competent and, therefore, as an adult, upon reaching the position of senior physician or opening their own practice—often not until well after the age of 30. The period of adolescence, that is, the time of change and transition, therefore lasts much longer. As a result, the overall group of adolescents has also grown larger.
CHANGE AS A CENTRAL PRINCIPLE OF ADOLESCENCE AND THE BIO-PSYCHO-SOCIAL APPROACH
Change defines adolescence and is the central principle of this stage of life, which begins with the onset of physical pubertal development and ideally ends with full independence from the parental home and integration into adult society. Adolescence thus encompasses all attempts to adapt to the new internal and external states brought about by physical pubertal development. I use the term “bio-psycho-social” to define the different levels on which changes occur. Here, “bio” refers to the physical level, “psycho” to the internal psychological processes, and “social” to relationships within the social environment. However, “bio-psycho-social” does not only define three separate levels—it also implies the mutual influence and interdependence among them. In this sense, considering the three levels separately is artificial and only justifiable for didactic purposes.
MORE
2.1. THE BIOLOGICAL LEVEL
Changes on the physical level are unmistakable. They are generally referred to as “pubertal development” and result from the increase in sex hormones.
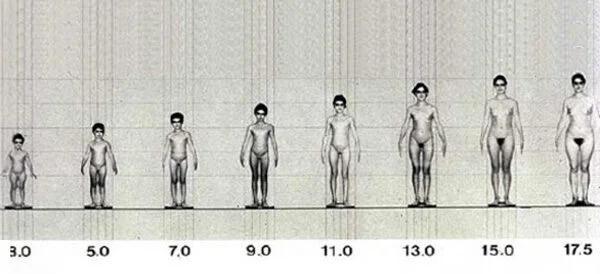
Figure 1 shows the physical changes of an average girl or young woman photographically. Between the ages of 3 and 11, the body remains largely unchanged except for growth in size. Between 11 and 15, the body undergoes fundamental changes in addition to growth.
Pubertal development in girls begins with breast development, the appearance of pubic hair, and a growth spurt, typically around the age of 11. Menarche usually occurs at about 13 years, and by age 15 growth is complete and regular fertile cycles become established. In boys, puberty generally begins around age 13 with testicular enlargement and the appearance of pubic hair. Between ages 14 and 15, the pubertal growth spurt reaches its peak, the voice breaks, and the first ejaculation occurs. By age 17, growth and pubertal development are complete.
2.2. THE PSYCHOLOGICAL LEVEL
The intrapsychic level is characterized by the emergence of new, previously unknown feelings, which are partly rooted in the altered hormonal situation (pubertal increase in sex hormones) and partly in the fundamental changes in physical appearance. The physical changes are initially experienced as unfamiliar (“it is happening to me”) and must subsequently be integrated into a new internal self-image. These bodily changes are perceived both directly and indirectly, through the reactions of the surrounding environment. This includes the responses of peers, as well as adults, caregivers, and strangers. For example, consider how the attention of adults toward a 13-year-old pubertal girl differs compared with that toward an 11-year-old prepubertal girl.
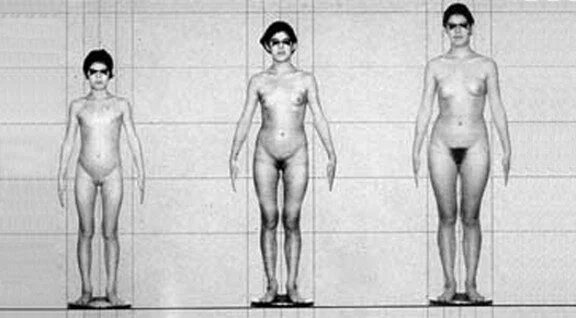
Figure 2 shows a section of Figure 1. Within four years, a child’s body transforms into that of an adult woman. The unity that existed for many years between the child’s body and mind (known in developmental psychology as the latency phase) must be reestablished on a new level—first as an adolescent, then as an adult. This new appearance must be integrated into a new internal self-image. The goal of all these efforts is to give the adult body a corresponding mature and fully adult self-image. As an example of a disrupted self-image, anorexia can be cited, characterized by the typical alienation from one’s own body.
2.3. THE SOCIAL LEVEL
Changes in the physical and intrapsychic domains are accompanied by changes in relationships with the social environment, where a new sense of autonomy must be established. The path to developing this autonomy typically and necessarily involves a phase in which dependence on the family of origin is gradually replaced by a new dependence on peer groups.
With the onset of physical puberty, adolescents begin moving out of the family and into groups of peers and like-minded individuals. Integration into these peer groups is essential for the transition out of the family to succeed. This process, in turn, is unavoidable if a child is to grow into an adult capable of independent thought and responsible action.
The social rules of peer groups—from school classes, youth groups, and scout troops to punks and skinheads—differ fundamentally from those of adults. In all these very different adolescent groups, conformity with other group members is the central requirement for being accepted. Physical maturity plays a key role in establishing hierarchy. Red-haired, overweight, and short-statured adolescents, to name just a few examples, often begin to struggle with their “nonconformity” at this age. The same is true for excessively tall adolescents. The need for conformity and uniformity is also reflected in clothing choices. Conformity and uniformity allow individuals to merge into the group and “disappear” within it, similar to the family structure. However, the highly uniform, identical outfits of certain youth subcultures (punks, Teddies, skinheads, etc.) carry an additional meaning. During this period of intense change, uniform dress serves as an external symbol signaling: We are all the same, there are no differences, nothing changes.
For us physicians, it is somewhat surprising to note that at this age, physical maturity is assessed less by body shape and mainly by height, even though this fact is well-supported by studies. We are used to examining our patients, sometimes partially undressed, which provides clear information about their developmental status. Outside the examination room, such information is not as easily accessible, and adolescents’ age-appropriate need for conformity leads them to dress accordingly. They protect themselves within peer groups by using clothing to simulate a certain level of maturity. Physicians focused on somatic care tend to underestimate the importance of physical expression through clothing.
NEEDS FOR ADOLESCENT-ORIENTED MEDICINE
Here, too, I like to use the term “bio-psycho-social” as a guide, or rather as a framework.
3.1. THE BIOLOGICAL LEVEL
Being knowledgeable and competent about the physical changes of puberty, and being able to judge what is still normal at each age, seems essential. A physician must therefore be able to answer questions such as: Is my height normal? How tall will I be as an adult? Could treatment make me taller? Are all my organs normal and functioning properly? Are my breasts too small? Are they still developing, will they grow more? Is my penis normal, not too short for my age, will it continue to develop? I have developed breasts; am I still a “real” man? Could it be cancer? Is my physical development truly delayed? Will it still progress, or should I be concerned? Could it be medically accelerated? Is my body hair normal? I have not had my period yet, or my period is absent; should I worry? I am afraid of AIDS, pregnancy, etc. Many questions arise from the situation of change. What was normal yesterday may be different today. This requires ongoing engagement with the changes in one’s body, the shifting concept of what is normal, and ideals of how a male or female body should look. Knowing the uncertainty adolescents feel about their physical changes and the many questions that arise also carries the risk of providing reassurance too quickly, potentially overlooking medically relevant findings (e.g., hypogonadism versus delayed puberty). A physician should be able to distinguish normal from pathological features at every age. This requires solid medical training and experience with adolescents.
MORE
The example of secondary amenorrhea in young women illustrates well how complex differential diagnosis can be in adolescents, involving multiple levels. A missed period at this age may be physiological, reflecting an immature and irregular cycle. This instability can be exacerbated by psychological or physical stress. In some cases, the first bleeding may not even have been menarche, i.e., not of uterine origin. Therefore, the patient’s overall maturation status must be assessed and bone age determined. Amenorrhea can be the first symptom of anorexia and often occurs before weight loss. It can also result from anorexia and sometimes persist for years even after normal weight is achieved. Any type of chronic illness can lead to amenorrhea. It may also be caused by pregnancy or hormonal disorders, particularly dysfunctions of the thyroid, ovaries, adrenal glands, pituitary, or hypothalamus. It is, of course, not possible to formally exclude all these differential diagnoses, as many complex and poorly understood diagnostic procedures at this age can themselves provoke anxiety and potentially have harmful effects. This example clearly demonstrates that the problems for which adolescents consult a physician are quite different from those of other age groups. In addition to the problem areas listed above in question form, adolescents frequently present with eating disorders such as anorexia nervosa, obesity, and bulimia.
3.2. THE PSYCHOLOGICAL LEVEL
In the psychological domain, the focus is primarily on helping adolescents overcome the temporary disintegration of body and mind and integrate their changed, new body into a stable and consolidated self-image. At this age, this creates a particularly strong need for holistic medicine. Medicine that is divided into somatic and psychological branches makes this integration more difficult for adolescents. In particular, psychosomatic illnesses in adolescents often originate from this disintegration. Anyone working with adolescents engages in psychotherapeutic work more frequently than they might realize. Adolescents will only consult a psychiatrist or psychologist in extreme cases (“I’m not crazy”). Approaching a physician through a somatic symptom is usually an easier path for them.
MORE
Certain qualities such as honesty, transparency, flexibility, and availability facilitate contact and building a relationship with adolescents. One should be willing to learn from them and open enough to question oneself and reconsider one’s own positions. Often, we serve as a model. Sometimes we take on the role of mother or father, especially when one parent is physically or psychologically absent, or perceived as weak. We cannot truly replace these roles, but we can make ourselves available, acting like a projection screen for the image the adolescent projects onto us. Due to these specific demands, the psychological expectations of the treating physician are quite high. Psychological and psychotherapeutic aspects are often underrepresented in medical education. Anyone working with adolescents must acquire the necessary competence in this area. Continuing education in the form of Balint groups represents an absolute minimum. For therapeutic work with children and adolescents under the concept of “holistic” or “psychosomatic” care, training in family therapy is recommended to understand different systems (family, school, etc.) and intervene competently if necessary. Furthermore, I consider personal therapeutic experience essential. It is feasible for a practicing physician to obtain such training. Several well-qualified institutes offer programs that can be completed alongside daily clinical practice. Such training often includes at least partial supervision, allowing physicians to work psychotherapeutically in practice from the start.
3.3. THE SOCIAL LEVEL
Regarding the adolescent’s social environment, there are primarily two expectations for the physician. First, the physician should understand the rules to which adolescents are exposed and subject within their peer groups. Second, the physician should be able to support the adolescent in the pursuit of autonomy. In cases of family or school conflicts, it can be helpful and appropriate to conduct family meetings or meetings with the parents alone. However, supporting the adolescent’s autonomy is often less a matter of teaching and more a matter of direct demonstration through the physician–patient relationship in the here and now. The physician helps the adolescent develop autonomy by allowing them to reduce their dependence on the physician. This can serve as a model for reducing dependence on their parents. Physicians should enjoy explaining and, in this way, help the adolescent take ownership of their body and understand its functions. For example, in the past, diabetologists required patients to call the doctor for every change in blood or urine sugar, who then instructed them on how to adjust insulin doses. Today, fortunately, most patients learn to manage their lifelong condition themselves and adjust insulin doses independently according to their needs. The former approach kept patients dependent, while the latter allows patients to act autonomously and responsibly.
04. SUMMARY
Adolescents represent a distinct and increasingly large patient group. The central principle of puberty and adolescence is change, which requires continuous engagement with a constantly shifting sense of normality. Changes occur on the physical, intrapsychic, and psychosocial levels. This situation of ongoing change demands specific knowledge and skills from physicians. These skills are derived in part from pediatrics, endocrinology, andrology, gynecology, as well as psychology and psychiatry. Specialized adolescent physicians are therefore needed. Such specialists are not only essential for working directly with adolescents but also to share their expertise and experience in the training of students and colleagues.
Prof. Dr. Urs Eiholzer

ADOLESCENT MEDICINE IN THE PRACTICE
FOR A “HAPPY” UPBRINGING
In my professional experience, I quickly realized that current medical care practices do not adequately address the needs of adolescent patients. However, I believe that responding to adolescents and their physical and emotional development is essential for a “happy” upbringing.
01. ADOLESCENT MEDICINE AND DISEASE
“Adolescents aren’t ill,” I was told ten years ago by the pediatric establishment when I spoke about my interest in adolescent medicine and my thoughts on the medical care of young people. The statement “Adolescents aren’t ill” holds true only if one adopts a very narrow definition of disease. How severe does acne have to be before it can be considered an illness? Is pubertal gynecomastia a disease?
MORE
Is the fact that one suffers from it a disease? What about delayed menarche, irregular menstrual cycles, or the fear of not developing normally, or that one’s genitals are too small or too curved? Is the desire for personal counseling about contraception a disease? Adolescents’ “illness” often lies in their distress. Young people are frequently worried, and in a way that affects both their well-being and their ability to function. This distress usually stems from the constant changes adolescents face in their daily lives. Profound transformations occur on three levels, commonly described as biological, psychological, and social. Many questions arise from these biological changes. What was normal and familiar yesterday may feel different today. This requires an ongoing process of adapting to change and to a shifting sense of what is “normal” in one’s own body. On a physical level, adolescents repeatedly ask themselves: are the changes they notice normal or abnormal (for example, increased body hair or a lack of pubertal development when peers have already begun puberty)? The body, which is evolving toward its adult form, is constantly measured against internalized ideals of what a “perfect” female or male body should look like.

On the intrapsychic level, there is often a relentless confrontation between the growing awareness of one’s own limitations and shortcomings and imagined ideals: body shape, proportions, height, breast size, penis size, as well as educational opportunities, future social status, athletic abilities, and more. Feelings of sadness, and sometimes even despair, arise when these idealized images have to be let go.

On the social level, the focus is on developing autonomy, as well as on acceptance and integration into peer groups and like-minded communities (moving away from the family and toward peer groups).
In the treatment of adolescents, the focus is often primarily on psychosocial aspects, even when a somatic complaint appears to be the main reason for consulting a doctor. Physical symptoms are chosen, first, because adolescents often lack the experience to recognize psychosocial problems as such; second, because the body is an important means of expression for children and adolescents; and third, out of fear of not being taken seriously by a physician if they do not present a physical complaint. Only adults tend to say that they feel unwell or depressed. Adolescents, by contrast, often communicate the underlying issue only in subtle ways. A physician can understand these cues only if they are familiar with the somatic, intrapsychic, and social processes of maturation.
02. PEDIATRICS AND ADOLESCENT MEDICINE
It is very important to us that adolescent medicine remains an integral part of pediatrics. But why are pediatricians particularly well qualified to care for adolescents?
First, pediatricians have usually known their patients since early childhood. A relationship is therefore already established and does not need to be painstakingly built from scratch. However, adolescents will continue to see their pediatrician only if the physician has learned to adapt the relational approach to the child’s or adolescent’s age and developmental stage. Pediatricians generally also have the trust of the parents.
MORE
This is especially important during the years of separation, because it is difficult for parents to relinquish control over their adolescent’s relationships. They manage it better if they know that their son or daughter can always turn to someone in difficult situations who also has their trust. It should be noted, however, that adolescents must be able to rely at all times on their physician’s confidentiality, even with regard to their parents.
Which doctor should adolescents go to otherwise? Young people often fit poorly into “adult” practices (internists, general practitioners, gynecologists). They have not yet learned to behave appropriately—or “adult-like”—and to feel comfortable in the adult world. Adolescents need one thing above all: time. They need time to feel at ease. They need time to become aware of their concerns and to be able to express them. Sometimes these concerns do not become clear in the first consultation. Adolescents often need explanations more than examinations. For these and other reasons, they can easily become a disruptive factor in adult practices, creating a double temptation for the physician to focus on the parents rather than the adolescent. For the pediatrician, it is worth investing in this, because the workday becomes more engaging, diverse, and multifaceted—and because there is a significant “market” here.
03. THE EDUCATION CHALLENGE
It is not enough to hold the title “Specialist in Pediatrics and Adolescent Medicine” or to state in a mission statement that one feels responsible for patients beyond the age of 15 or 17, without also demonstrating the necessary competence. In pediatric training and continuing education, too little emphasis is placed on this, and there are too few opportunities to acquire the required skills.
MORE
A mission statement without corresponding training, continuing education, and professional development opportunities is not credible. Private initiatives are too often perceived as competition by institutions. Regarding adolescent medicine, however, the mission statement must face further fundamental criticism. The statement “With adolescents, conversations focus primarily on sexual behavior and addiction problems” does not align with the many years of experience of our practice group.
04. THE FUTURE
Some dark clouds are gathering on the horizon for adolescent medicine. Various health insurance models with restricted choice of physicians are likely to make it more difficult for adolescents to access a competent medical partner who meets their needs and makes them feel understood and taken seriously. The motivation of a physician working within such a model to refer patients is, by definition, not very high. Moreover, as noted at the outset, an adolescent’s “illness” is often perceived only as worry or uncertainty and seems, with remarks like “It’ll work out” or “Don’t take it so seriously,” to be relatively easily “treated.”
MORE
But this only seemingly solves the problem; the question is simply no longer asked. This is also not promising for addiction and suicide prevention, and ultimately represents money saved at a high cost. In general, adolescents are considered “low-risk” by health insurers because they use relatively few medical services. In doing so, however, the parents subsidize the medical care of the older population through the health insurance premiums of their children and adolescents. This situation obliges us, however, to ensure adequate medical care for adolescents. This means providing them not only with specialized knowledge but also with an appropriate framework tailored to their needs.
05. SOME CONCRETE SUGGESTIONS FOR THE PRACTICE
Doctors often define the scope of their practice through its appearance, particularly through the design of the waiting room. In many pediatric practices, the waiting room resembles a children's playroom, making it clear that adolescents may feel out of place. It is therefore advisable, for example, to create separate areas in the waiting room for different age groups and to put away or set up toys before adolescent clinic hours. This brings us to the next point: different age groups should be scheduled in fixed time blocks, resulting in dedicated clinic sessions for infants, older children, and adolescents.
MORE
Infants and toddlers can easily be scheduled in the morning. Specific afternoons can be reserved for school-aged children, and other afternoons or early evening hours for adolescents. Pediatric practices should also keep buffer slots available for emergencies so that adolescent consultations are not disrupted by crying babies and toddlers. Such a system has the added benefit of minimizing waiting times for patients. It not only signals to adolescents that they are respected as equal partners whose time is valued, but the use of dedicated time blocks for different age groups offers another important advantage: communication styles vary significantly depending on the patient’s age. With infants, the consultation takes place exclusively with the mother or father. As the child grows older, the focus of the conversation increasingly shifts toward the child rather than the accompanying parents. Constantly adjusting this level of communication between patients can be very challenging.
With adolescents aged 12–13 and older, it is advisable, whenever possible, to speak with them first on their own, that is, without their parents present. This conveys a clear message: you are my patient and my conversation partner—not your mother or your father. I want to listen to you first and understand what you would like from me. At the beginning of the consultation, questions such as the following should be asked: Why are you coming to see me? What would you like from me? What do you expect from me so that you can leave here feeling satisfied?
Being knowledgeable and competent about the physical changes of puberty, and being able to judge what is still normal at each age, seems essential. A physician must therefore be able to answer questions such as: Is my height normal? How tall will I be as an adult? Could treatment make me taller? Are all my organs normal and functioning properly? Are my breasts too small? Are they still developing, will they grow more? Is my penis normal, not too short for my age, will it continue to develop? I have developed breasts; am I still a “real” man? Could it be cancer? Is my physical development truly delayed? Will it still progress, or should I be concerned? Could it be medically accelerated? Is my body hair normal? I have not had my period yet, or my period is absent; should I worry? I am afraid of AIDS, pregnancy, etc. Many questions arise from the situation of change. What was normal yesterday may be different today. This requires ongoing engagement with the changes in one’s body, the shifting concept of what is normal, and ideals of how a male or female body should look. Knowing the uncertainty adolescents feel about their physical changes and the many questions that arise also carries the risk of providing reassurance too quickly, potentially overlooking medically relevant findings (e.g., hypogonadism versus delayed puberty). A physician should be able to distinguish normal from pathological features at every age. This requires solid medical training and experience with adolescents.
A final word on medical confidentiality: adolescent patients should be explicitly informed that medical confidentiality also applies in relation to their parents. No information from the medical history or examination is shared with parents without the adolescent’s explicit consent. If parents wish to speak with me about their son or daughter, I usually ask the adolescent whether they would like to be present and represent their own point of view. There may occasionally be exceptions. What is important is that adolescents are not denied the opportunity to make decisions concerning themselves and to take responsibility for their own lives.
06. TWO TYPICAL EXAMPLES
The following two examples are intended to illustrate the complexity of adolescent medicine and, in particular, to highlight how high the demands on the treating physician can sometimes be and how essential well-structured continuing education is.
MORE
Hirsutism is a fitting example to illustrate the demands placed on a holistic approach in adolescent medicine. This condition—excessive body hair growth in females—most commonly occurs during pubertal development. Regardless of whether the increased body hair represents a normal variation or an underlying pathological condition, it is experienced by the affected young woman as something new and therefore at least in need of explanation, if not of further evaluation and treatment. However, hirsutism is not only a physical concern; it also affects the integration of the changing body into a new self-image, which during adolescence is often shaped by an idealized and imagined “perfect” body. The ideal female body, as portrayed for example in magazines, is currently depicted as almost hairless. Furthermore, hirsutism can be distressing because it is perceived as a “nonconformity” and may expose the individual to peer pressure (e.g., “You have a moustache”).
Physicians who specialize in adolescent care should be able to address these considerations appropriately—that is, in a therapeutic manner—within an explanatory discussion with the patient. However, this alone is not sufficient. Hirsutism may also be a sign of an underlying medical condition (e.g., adrenogenital syndrome, adrenal cortical adenoma, or polycystic ovaries), and such conditions must be reliably ruled out. Even when hirsutism represents a normal variation, it can be sufficiently distressing to justify medical treatment in addition to cosmetic measures. Here, too, appropriate expertise and clinical knowledge are essential.
Another typical example is short stature, which particularly affects adolescent boys around the age of 12 to 13. Being short at this stage of development is often experienced as difficult and distressing. As a result, physicians frequently encounter this issue in this age group. The main concern is the emotional burden caused by difficulties in gaining access to peer groups. Short stature conflicts with the need for conformity and is further disadvantageous because being short is often associated with immaturity. Within these peer groups, it is linked to a lower social status and reduced acceptance.
Als behandelnde Ärzte sollten wir in der Lage sein, zuerst einmal ein pathologisches Geschehen als Ursache des Kleinwuchses auszuschliessen. Wenn der Kleinwuchs einmal als Normvariante identifiziert ist, stellt sich die Frage nach den zur Verfügung stehenden Behandlungsmethoden. Diese reichen von der einfachen Berechnung der voraussichtlichen Erwachsenengrösse aufgrund des Handröntgenbildes und der Erklärung des erwarteten Wachstumsmusters (beispielsweise konstitutionelle Verzögerung von Wachstum und Pubertät) bis hin zu einer Hormonbehandlung (beispielsweise mit niedrig dosiertem Testosteron).
Understanding the significant emotional burden that can arise from constitutional delay helps to provide effective guidance and counselling to the patient.
SUMMARY
Adolescents represent a distinct and growing group of patients. The central principle of puberty and adolescence is change, which requires continuous adaptation to ever-evolving norms. These changes occur on physical, psychological, and psychosocial levels. This state of constant change demands specific knowledge and skills from physicians. These are drawn in part from pediatrics, endocrinology, andrology, and gynecology, as well as from psychology and psychiatry. Pediatricians are particularly well suited to care for adolescents. However, they must acquire additional competencies, as current training in pediatrics still tends to focus too heavily on hospital-based needs, where the specific needs of adolescents often receive insufficient attention. From our experience, it is clear that this additional effort is worthwhile for pediatricians, as it makes their work more diverse and multifaceted. It is fascinating to witness how a child develops into a confident adult.
Prof. Dr. Urs Eiholzer
ADOLESCENT MEDICINE
INTERDISCIPLINARY COLLABORATION IS PARTICULARLY IMPORTANT IN ADOLESCENT MEDICINE.
In the emerging paradigm shift in pediatrics, adolescent medicine is becoming increasingly important. This raises new questions regarding medical care. Dr. Eberhard Zangger from PÄDIATRIE magazine, spoke with pediatric and adolescent specialist Prof. Dr. med. Urs Eiholzer, who runs a large group practice in Zurich.
INTERVIEW
PEDIATRICS: Dr. Eiholzer, why do you advocate for comprehensive, interdisciplinary care for young patients?
Eiholzer:During my time as a pediatric endocrinologist at the Zurich Children’s Hospital, I realized that a university hospital is rarely the ideal setting for providing comprehensive care to patients. In such large-scale environments, the emotional aspects of illness are often overlooked. In many cases, organic diseases in children and adolescents are closely linked to psychological issues. It is also quite common that no organic condition is present at all; for example, some children simply feel that they are too short and suffer because of it. These patients are more likely to require psychological support. Adolescent medicine must therefore, by necessity, adopt a psychosomatic approach. For me personally, this insight led me to further deepen my training in psychosomatic medicine. After establishing my own practice and once patient numbers allowed, I brought a therapist into the team. Today, this has developed into an interdisciplinary team of six specialists.
MORE
PEDIATRICS: Is a group practice more than just a “geographical grouping” of individual practices?
Eiholzer:In outpatient care, treatment is often fragmented: the physician treats, the psychologist treats, and other specialists provide their own care as well. Each speaks a different “language,” and what they often have in common is that the patient does not fully understand them. The main difference between such an approach and the care we provide in our group practice is quite simple: communication here is far more efficient. The short distances—what you refer to as a “geographical grouping” of practices—ultimately offer a decisive advantage. Through brief and frequent exchanges between colleagues, often in passing, many emerging issues can be resolved quickly and easily. For example, when a girl enters puberty too early, the question arises whether the process should be slowed down. Such a case requires discussion between the physician, the psychologist, the patient, and the family. We are able to do this without significant effort. In addition to physical proximity, it is also crucial that team members have a broad base of knowledge, are able to understand each other’s perspectives, and maintain a relationship of mutual trust. In our setting, close collaboration fosters respect for each other’s work. This helps us avoid unproductive rivalries and conflicts, creating a positive atmosphere that ultimately benefits patient care.
PEDIATRICS: Your patients sometimes need to talk about very personal matters. Isn’t it difficult to build trust with several people?
Eiholzer:Of course, it is more difficult for patients to open up to several people. However, when interdisciplinary care is essential—for example, when both physical and psychological aspects of illness are involved—it is easier for patients to confide in specialists working within the same setting. A major advantage for patients is also the minimal friction between therapists. The physicians and psychologists in this practice do not compete with one another. As a result, referrals between colleagues who work well together are generally successful.
PEDIATRICS: How do patients find out about you?
Eiholzer:Many children come to us with growth and puberty-related concerns. About two-thirds of our patients are referred to us by physicians outside our practice, including private pediatricians. In these cases, the referrals often involve unclear diagnoses or uncertainty as to whether the patient is suffering from a hormonal or psychological issue. In many instances, we are simply required to provide clarification and guidance.
PEDIATRICS: WHAT KIND OF PATIENT POPULATION DO YOU TREAT OVERALL?
Eiholzer:Many children and adolescents struggle with school-related worries and anxiety. Some have specific learning difficulties and/or are either over- or underchallenged. In most cases, existing growth disorders also affect their appearance. These children are often too small, too tall, overweight, or underweight, which can cause further problems for them. We see children who wet the bed in the prepubertal stage as well as adolescents whose development into adulthood seems to stall because they are unable to separate from their families. In addition, there are children with physical or intellectual disabilities. Our comprehensive care approach means that these children undergo thorough assessment so that each individual can be guided toward the most suitable school placement, education, and career path. In some cases, care continues over many years. We also offer psychotherapeutic support for adult patients.
PEDIATRICS: HOW HAS THE COMPOSITION OF THE TEAM CHANGED OVER TIME?
Eiholzer:From the very beginning, we have offered a broad range of services. Our goal was to achieve greater depth in our offerings by bringing in additional specialists. In the meantime, our team has become an internationally recognized research institute for questions related to growth and puberty.
PEDIATRICS: WHAT ARE THE IMPLICATIONS OF INTERDISCIPLINARY WORK FOR PATIENT CARE? WHAT CHANGES CONCRETELY COMPARED TO TREATMENT IN A SOLO PRACTICE?
Eiholzer:Treatment does not follow a fixed scheme; it varies from case to case. For example, a child with a growth hormone deficiency is short and requires hormonal treatment. At the same time, the question arises of when to enroll the child in school. The teacher may feel that the child should attend a special school. The parents believe the child is bright, and the kindergarten teacher suggests keeping the child in kindergarten for another year. With average intelligence, about 50 percent of children who are too small start school a year later than usual. As a result, the child not only faces the disadvantage of being short but is also artificially given the additional disadvantage of not being allowed to prove themselves. This must be avoided at all costs. In such cases, we carry out a comprehensive assessment. We want to understand what the child is capable of, how they feel, and how mature they are. Ultimately, the parents then work with the educational authorities to find the best possible solution based on our assessment.
PEDIATRICS: WHAT IS THE VIEW OF HEALTH INSURANCE PROVIDERS ON INTERDISCIPLINARY CARE? IS AN “EIHOLZER PATIENT” NOT TWICE AS EXPENSIVE AS A PATIENT SEEKING TREATMENT IN A SINGLE-DOCTOR PRACTICE?
Eiholzer:Over the 15 years since our group practice was established, not a single invoice has been disputed by health insurance providers. This is probably not a bad sign. It is also likely clear to insurers that well-coordinated multidisciplinary care for a patient is more cost-effective than the poorly coordinated process of moving from one specialist to another. Within our group practice, each specialist essentially acts as their own employer. This means that each specialist also bills their services independently. Where hierarchies exist, we strive to keep them as flat as possible. We have highly qualified psychologists who, ideally, would operate as a self-contained team to the outside world. However, legally, delegated psychotherapy is bound by strict regulations and depends both on medical referrals and on ongoing medical supervision of the patients. This creates certain internal dependencies. For this reason as well, close collaboration between physicians and psychotherapists is essential.
PEDIATRICS: HOW IS YOUR GROUP PRACTICE ORGANIZED? ARE YOU NOT MORE OF AN ENTREPRENEUR AND MANAGER THAN A PHYSICIAN?
Eiholzer:This is a serious issue. The amount of administrative work involved should not be underestimated. In addition to routine administration, there is also public relations, the planning and delivery of continuing education, setting up and maintaining a website, and similar tasks. Moreover, in our case, one person bears the majority of the entrepreneurial risk. Financially, our practice is based on a mixed-cost model, which provides us with a solid foundation.
PEDIATRICS: YOU MENTIONED PUBLIC RELATIONS. IS THIS AN INTEGRAL PART OF YOUR APPROACH?
Eiholzer:We cannot take on more patients than our available capacity allows. That is why we try to share the experience we have gained here with others—both with specialists and with those directly affected, namely patients and their families. For example, we organize workshops and support self-help groups. Ultimately, our goal is to help as many patients and affected families as possible, going beyond our day-to-day clinical work.